IN the rush of our daily lives, we can be ignorant to the markers of our health that don’t get in the way or slow us down. One of the most critical is blood pressure.
Many patients are surprised to discover their readings are high because they feel perfectly fine.
 Dr Zoe Williams answers this week’s health questions from readers – from painful ejaculation to vertigo treatment Credit: Olivia West
Dr Zoe Williams answers this week’s health questions from readers – from painful ejaculation to vertigo treatment Credit: Olivia West
This is why is often referred to as a “silent killer” – it puts strain on your heart and blood vessels without warning.
Statistics show that more than 14 million adults have high blood pressure, and as many as five million of those are undiagnosed. Untreated hypertension significantly increases the risk of heart attack, and kidney disease.
To keep blood pressure (and heart) healthy, try to reduce your salt intake and aim for at least 150 minutes of moderate activity a week.
Also take advantage of the free blood pressure checks offered at most high street pharmacies. If your readings are consistently above 140/90mmHg, book an appointment with your .
Here’s what readers have been asking me this week . . .
- Got a question for Dr Zoe? Email her at health@thesun.co.uk
Going round in circles over spreading spots
Q: IN March 2025, I developed itchy red spots on my back that spread to new parts of the body every day. Various prescription creams didn’t help.
By May, they were at their worst and all getting crusted over.
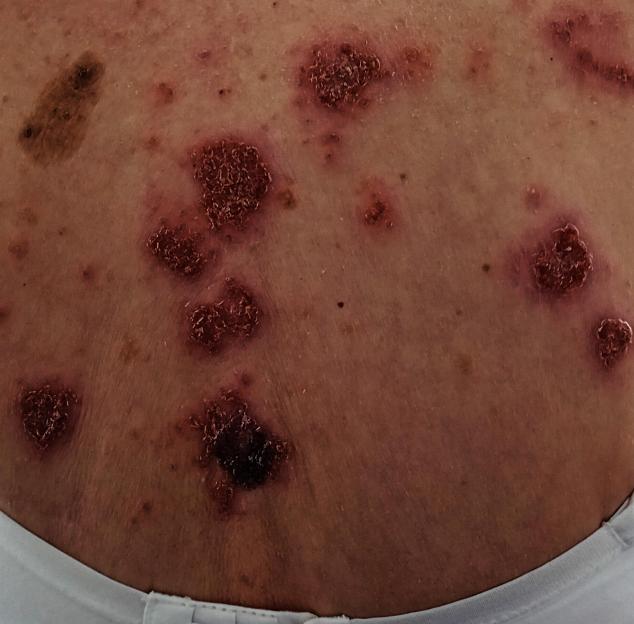 A reader’s spreading red spots are itchy and all crust over – but she’s had multiple diagnoses Credit: Supplied
A reader’s spreading red spots are itchy and all crust over – but she’s had multiple diagnoses Credit: Supplied
I asked for a lupus blood test because I had fatigue, a butterfly rash on my face and a burning sensation across my forehead.
The blood test result was inconclusive, but while one doctor said I had , a rheumatologist said I did not and that it was vasculitis.
A dermatologist said it was and that I didn’t need a biopsy.
I am a woman of 86 and I had a stroke two years ago.
A: Thank you for sharing some very helpful photos with me, including the one here. What’s visible on the picture are multiple inflamed, red lesions, some of which have become crusted and ulcerated, alongside areas that are healing with flat, pink or pigmented patches.
That pattern – active inflamed spots plus healing marks – suggests a recurrent inflammatory skin process rather than a simple, one-off rash.
It does not look like eczema alone, given the severity, widespread distribution, the cycle of flare and healing and your systemic symptoms.
But having said that, it might have looked like eczema at the time you saw the dermatologist.
A skin biopsy is key here – without one, you’re essentially guessing. There are a few possibilities that doctors would be considering.
These include cutaneous vasculitis, autoimmune/connective tissue disease, a medicine-related skin reaction and, less commonly, certain blistering or inflammatory skin disorders of later life.
The fact this has been ongoing, severe and is unresolved means it absolutely warrants specialist dermatology input with biopsy, not just creams.
Ask your GP for an urgent dermatology review, requesting a biopsy of an active lesion. Be sure to attach your photographs to the referral.
PAINFUL PLEASURE
Q: I’M a 70-year-old man. When I ejaculate, I get an unbearable stabbing pain in my hips. It’s embarrassing as well as very painful. Is there a reason?
A: That does sound both painful and understandably embarrassing, but it’s a recognised symptom and there are some plausible explanations.
Pain on ejaculation – sometimes called orgasmic or ejaculatory pain – is most often linked to the prostate, pelvic floor muscles, or nearby joints and nerves.
One common cause is prostatitis (inflammation of the prostate), which can cause pain during or after ejaculation, sometimes felt deeper in the pelvis, lower back, or even into the hips.
This can occur even without obvious urinary symptoms.
Another possibility, particularly given your description of stabbing pain in the hips, is a musculoskeletal or nerve-related cause.
During ejaculation, there are strong pelvic muscle contractions, and if there is any underlying hip arthritis or nerve irritation, or if there are lower spine issues, this can trigger sharp, referred pain into the hips.
There are also several other potential, less common causes, such as other prostate problems, spasms of the pelvic floor muscles, or nerve irritation in the lower spine or pelvis.
The key point is that pain that is only occurring at ejaculation suggests a mechanical or functional trigger, rather than something that is constantly inflamed.
It would be a good idea to see your GP, who may wish to assess your prostate, do a urine test to exclude infection and consider whether musculoskeletal or spinal issues could be contributing to the pain.
In many cases, once the underlying cause is identified, treatment – whether it will be medication, physiotherapy or addressing prostate inflammation – can make a significant difference.
This is a sensitive health problem, but a very valid one to raise, and there are potentially treatable causes that are worth exploring.
Should I try Epley method at 86 to fix vertigo?
Q: I AM an 86-year-old man and, ten days ago, I started getting , which I’ve never had before. It’s much worse when I lie down and then go to get up.
My GP said that everything was fine, including my blood pressure. Prochlorperazine did not help.
The GP also said that I only looked about 60, which I put down to being married to a wonderful lady for 66 years. Should I try the Epley manoeuvre?
 An 86-year-old reader is struggling with vertigo over the past 10 days Credit: Getty
An 86-year-old reader is struggling with vertigo over the past 10 days Credit: Getty
A: It sounds as though you’ve been coping remarkably well and it’s lovely to hear about your long and happy , which certainly counts for a lot.
From your description – sudden onset , worse when lying down or getting up, with normal examination and blood pressure – this does sound very typical of benign paroxysmal positional vertigo.
This is caused by tiny crystals in the inner ear becoming displaced, which affects balance and causes brief spinning sensations with changes in head position.
Prochlorperazine can sometimes help with the nausea, but it doesn’t treat the underlying cause of BPPV – which is why it may not have made much difference to you.
The Epley manoeuvre, a series of head movements, is actually one of the main treatments for BPPV.
It works by guiding those crystals back into the correct position and many people find it very effective – sometimes even after just one or two attempts.
It’s generally safe for you to try, provided you feel steady enough, and there are some good demonstrations online.
Search “Epley NHS” to find the videos that I usually share with my patients for this.
Because you’re 86 and this is new, I would suggest doing it carefully and, ideally, with someone nearby in case you feel unsteady.
If your symptoms don’t improve after a week or two, or if you develop other symptoms such as persistent dizziness (not just with movement), double vision, weakness or difficulty walking, you should seek further medical advice.
But overall, your symptoms fit very well with BPPV, and the Epley manoeuvre is a reasonable next step.
Tip of the week
If you are a carer to a loved one, please prioritise your own health.
It should be documented on your medical record that you are a carer as it helps GP surgeries and hospitals be sensitive to this – such as considering appointment times or additional support.