UP to one in five Brits suffer with them, yet the solution remains elusive.
Many feel resigned to wear compression socks forever, or are stuck on an endless merry-go-round of visits and pricey, quick-fix ‘cures’. However, failing to treat varicose veins properly risks more than just an unsightly look – it could prove deadly.
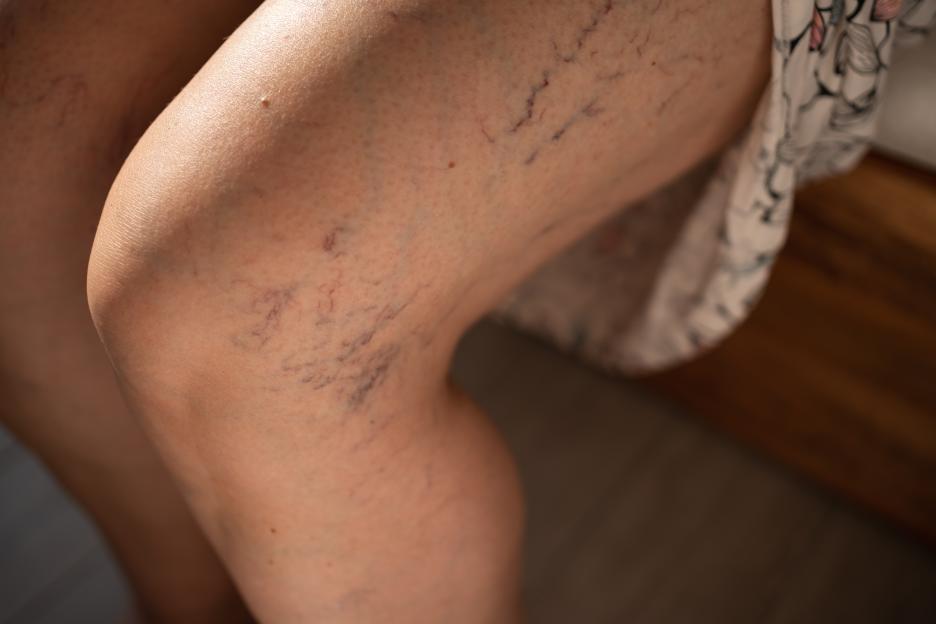 One in five Brits suffer with varicose veins, but they can lead to skin damage, clots, and debilitating ulcers if left untreated Credit: Getty
One in five Brits suffer with varicose veins, but they can lead to skin damage, clots, and debilitating ulcers if left untreated Credit: Getty
 Kate Lawler sought help after years of feeling self-conscious and avoiding bikinis because of her ‘blue cheese’ legs Credit: Getty
Kate Lawler sought help after years of feeling self-conscious and avoiding bikinis because of her ‘blue cheese’ legs Credit: Getty
Professor Mark Whiteley, founder of The Whiteley Clinic and the UK’s leading venous expert, tells Sun on Sunday Health: “This idea that varicose veins are just cosmetic was quashed 25 years ago.”
Left untreated, they can lead to aching, venous , skin damage, clots, and debilitating ulcers.
More alarmingly, there are links to some of the biggest killer conditions.
Prof Whiteley says: “If you don’t treat them, it worsens your risk of , and ischemic . If you treat the veins, the risks go back to negligible.”
A study in the journal PLOS One last year linked varicose veins with a 24% over 13 years, while the same team found a 17% higher risk of heart failure.
In his new book, Why Varicose Veins Come Back – And How To Stop Them! , Prof Whiteley sets out to debunk the many myths surrounding – including the idea that it’s your fault you have them.
While private clinics offer high-tech solutions, your GP should take the issue seriously, too.
RED FLAG WARNINGS
The NHS often views varicose veins as “usually harmless” unless they cause severe complications. Hate the way yours look?
Unfortunately, you’ll likely only be offered lifestyle advice – but this is still crucial to follow to avoid the problem worsening.
It includes exercising to keep blood flowing and maintaining a healthy .
However, if you experience pain, itching or swelling, you should push for a specialist referral.
You may have varicose eczema, which can lead to flaky, scaly or blistered or hardened (lipodermatosclerosis) skin or leg ulcers, which may take months to heal.
“Any aching or tenderness in your pelvis or lower legs… you should instantly think: ‘Is this venous disease?’” says Prof Whiteley.
“You should insist on a scan, because without a scan, you don’t know if you have varicose veins.”
A duplex ultrasound is the gold standard for diagnosis, as it reveals varicose veins not visible to the naked eye – and it shouldn’t be rushed in less than 20 minutes, Prof Whiteley says.
 Prof Whiteley sets out to debunk the many myths surrounding varicose veins Credit: The Whiteley Clinic
Prof Whiteley sets out to debunk the many myths surrounding varicose veins Credit: The Whiteley Clinic
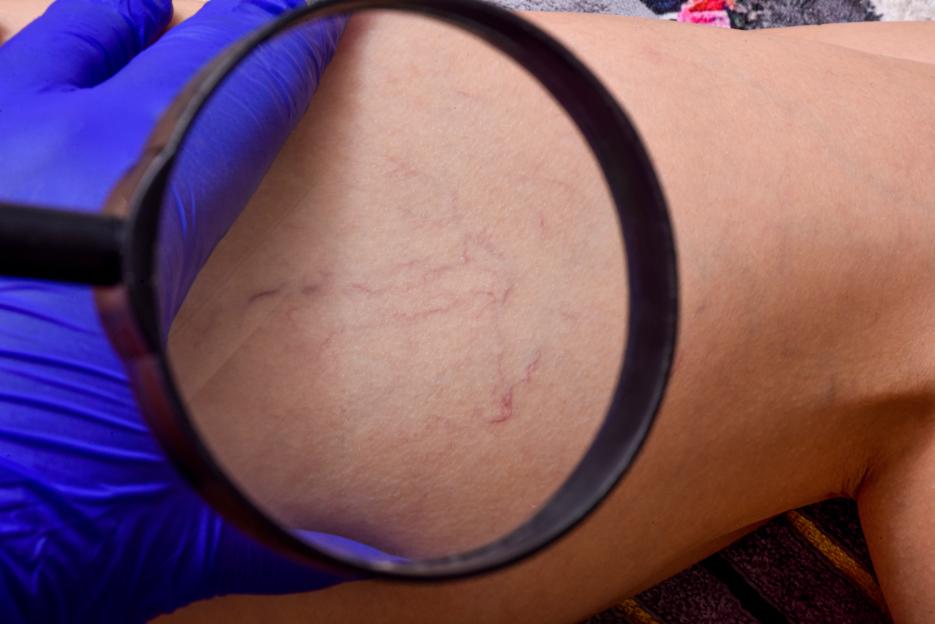 If you experience pain, itching or swelling, you should push for a specialist referral Credit: Getty Images
If you experience pain, itching or swelling, you should push for a specialist referral Credit: Getty Images
“People think there’s only two veins that cause when it’s been shown that only accounts for, at most, 15 per cent but probably five-10 per cent of cases.”
Modern treatments have moved beyond old-school surgery of stripping or ligation – though this is still offered as a last resort.
These days, the first-line options include endothermal ablation, which is when a laser heats the veins, closing them off and blocking blood flow, and foam sclerotherapy, a chemical solution that blocks blood flow.
Both procedures are done under local anaesthetic and require compression stockings for around a week of recovery.
Prof Whiteley says: “You should not accept steroids from your GP or stockings unless they’re saying, ‘We’re giving you this for now, because we’re going to get a duplex scan to find out how to cure you afterwards’.”
The treats varicose veins as a ‘wait and see’ condition, often only stepping in once there is damage, while Prof Whiteley takes a more preventative approach, to reduce accumulating damage.
He says: “If you get a proper scan and find all the causes, you use proper techniques, and you do the right operation for the right veins in the right order, your only risk of getting varicose veins back in the future is if you develop a new varicose vein.”
MYTHICAL CAUSES
IN his new book, Why Varicose Veins Come Back – And How To Stop Them, Prof Whiteley clarifies that varicose veins are entirely genetic.
'Blue cheese' legs
IT was during her thirties that first began to worry about her “blue cheese” legs.
After years of feeling self-conscious and avoiding bikinis, the 2002 winner sought help – and says her pins are now “like cheddar” again.
Ex-Virgin radio host, Kate, now 45, tells Sun Health: “I knew, looking at my mum’s legs, that mine were only going to get worse.
“I even tried covering mine up with leg make-up.”
The TV and radio presenter from London says her grandmother suffered “terribly” from leg ulcers – but the family never connected the dots.
“We went to dermatologists, GPs, skin consultants and no one could ever tell us what caused her leg ulcers,” she says.
It was only after going to The Whiteley Clinic that Kate learned it was a side effect of untreated varicose veins.
After a tailored plan involving laser treatment and sclerotherapy, Kate is now pain-free.
The mum-of-one says the local anaesthetic “was the most painful part” of her day surgeries.
Admittedly, private treatment is “not cheap”, but Kate says: “If you just leave it, it just accumulates. It gets worse and worse and worse.
“It’s like when people start with an untidy house, and then suddenly they’re on Britain’s biggest hoarders.
“I know that I’ve nipped it in the bud.”
He debunks common misconceptions:
LEG CROSSING
“ABSOLUTE rubbish,” says Prof Whiteley, adding it’s an old message that got confused.
“People would cross their legs for modesty and die of . Nurses would say, ‘Don’t cross your legs because of your veins’.”
This got misunderstood as causing varicose veins.
STANDING
“DO hairdressers, surgeons and get more varicose veins? They don’t.
“If they’ve got varicose veins, because it’s genetic, standing makes them worse.”
HOT BATHS
“YOU get people coming in and they show you a leg full of thread veins on one side, and say, ‘This is because I have hot baths’.”
Heat dilates veins, but healthy veins constrict afterward.
“The hot bath is irrelevant,” says Prof Whiteley.
BEING OVERWEIGHT
ANOTHER driver of worsening varicose veins, but not a cause.
People who don’t much have more venous stasis – slowed blood flow, causing blood to pool in the lower legs and ankles.
“You get complications earlier for the same amount of varicose veins,” says Prof Whiteley.
PREGNANCY
“IF you’ve got varicose veins already, makes them look worse.
“You have an extra two litres of blood, which makes the veins bulge more and dilate, and so they become apparent.”
CONSTIPATION
“We know that veins don’t come from the top of the legs.
“So this idea that something happens at the top, and then you get this domino effect, is upside down.”
GENDER
“A study by Vaughn Ruckley found 51 per cent of men and 49 per cent of women have venous reflux, or varicose veins.”