A WOMAN who discovered her husband was cheating was dealt an agonising diagnosis after thinking she was in the all-clear for an entire year.
Eileen McGill, from , went straight to her local sexual health clinic after she discovered her husband had been unfaithful.
 Eileen now patient advocate for Cervivor, a nonprofit that works to spread awareness about cervical cancer Credit: Supplied
Eileen now patient advocate for Cervivor, a nonprofit that works to spread awareness about cervical cancer Credit: Supplied
 Eileen (second from left) with with her children and their partners Credit: Supplied
Eileen (second from left) with with her children and their partners Credit: Supplied
Initially, the mum-of-four was relieved to find she tested negative syphilis, gonorrhoea and HIV.
But Eileen was then dealt a devastating blow just 12 months later following her annual smear test when she discovered she had tested positive for HPV (Human Papilloma Virus).
Despite being a common STI, it wasn’t included in the tests she had done the year earlier following her husband’s infidelity.
Missing the diagnosis meant that Eileen was diagnosed with vulvar cancer and cervical cancer in 2019.
Then in 2023 the mum was also diagnosed with anal cancer.
Eileen, who is a teacher, told the Tampa Bay Times she wants to help others avoid her distress, since a simple vaccine could have stopped the cancer from developing.
The mum had no idea the cancers were preventable with a quick and easy vaccine, but since she was already married with children, Eileen opted out of the jab as she thought she’d never need it.
Since then, the mum has had a hysterectomy as well as other treatments in a bid to tackle the cancer.
According to the NHS, more than 70% of unvaccinated people will get HPV.
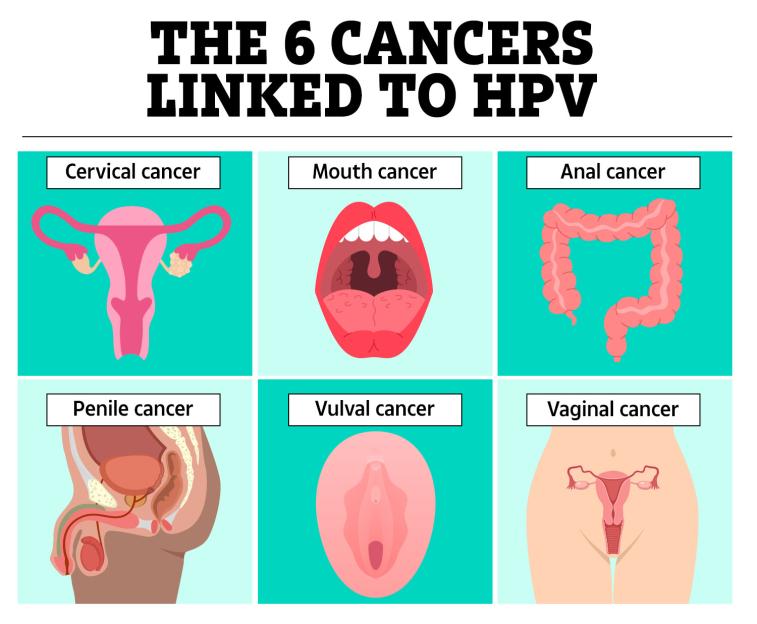
The common STI has been linked to six types of cancer, ranging from penile to mouth cancer.
Not only that, but most people who have HPV have little to no symptoms, meaning many don’t know they have it.
Now, Eileen wants to raise awareness and break the damaging stigma around HPV.
She said: “When I tell people I have anal cancer, I’m like, ‘It is what it is,’ let’s talk about vulvas and anuses and cervixes.
“Let’s remove the stigma and the shadow language for dealing with it.
“If it can happen to a married woman of 30 years, then it can happen to anybody,” she insists, saying even as a mother-of-four who devoted herself to others, she still found herself ‘on the receiving end of this vicious, vicious virus.”
Here in the UK, the life-saving vaccine that protects from the virus is offered to both boys and girls aged 12 to 13, with catch-up vaccines offered to people who missed it.
But the UK Security Agency (UKHSA) warned that over a quarter of eligible pupils are missing out on the life-saving jab each year.
The HPV vaccine has been offered to all girls in Year 8 since 2008, with Year 8 boys added to the programme in 2019 after evidence showed that it helps protect both genders from HPV-related cancers.
While people used to be offered two doses of the jab, nowadays only one is needed to offer protection from the virus.
The HPV vaccine has already reduced rates by 90 per cent in , and has reported zero cases in jabbed women since the programme began.
bosses reckon the jab will make cervical tumours the first kind of cancer to be completely wiped out, as HPV causes almost all cases.
Cancer Research UK’s chief executive, Michelle Mitchell, said: “The is clear: HPV vaccination is safe and effective.
“It’s vital that access to HPV vaccination and cervical screening is improved to ensure more lives aren’t lost to cervical cancer.
“I encourage all eligible people to take up these life-saving offers.”
“Every year, around 3,300 people are diagnosed with cervical cancer in the UK.
“Thanks to the power of research and efforts of NHS staff, we can eliminate cervical cancer as a public health problem in our lifetime – the HPV vaccine combined with cervical screening can help to bring about a future virtually free from the disease.”
EVERYTHING TO KNOW ABOUT THE HPV VACCINE
The HPV vaccine protects against some of the risky HPV types that can lead to genital warts and cancer.
Gardasil has been the HPV vaccine used in the NHS vaccination programme since 2012. It is protective against nine types of HPV.
For example it is effective against types 16 and 18 which cause around 80 per cent of cervical cancers in the UK.
That’s why it is important for people who have a cervix to still get a when invited by the NHS.
Cervical cancer takes the lives of 854 people a year currently – but this is expected to continue decreasing thanks to the vaccine.
There are around 3,200 new cases of the devastating cancer a year, with peak incidence in women in their early 30s.
But the HPV vaccine doesn’t just prevent cervical cancer – it stops some anal, genital (vaginal and penile), mouth and throat (head and neck) cancers.
These affect both men and women.
Who should take it?
The first dose of the HPV vaccine is routinely offered to girls and boys aged 12 and 13 in school Year 8.
The second dose is offered 6 to 24 months after the 1st dose.
If a school child misses their doses, you can speak to the
school jab team or GP surgery to book as soon as possible.
Anyone who missed their jab can get it up to their 25th birthday.
But people who have the first dose of the HPV vaccine at 15 years of age or above will need to have three doses of the vaccine because they do not respond as well to two doses as younger people do.
The HPV vaccine used to only be given to girls who are at risk of cervical cancer when they are older.
But in 2018, it was – who can get HPV-related cancers of the head, nech, anal and genitals – would also be given a jab.
Girls indirectly protect boys against HPV related cancers and genital warts because girls will not pass HPV on to them.
But the programme was extended to further eliminate risk of the virus spreading in the future.
Men who have sex with men (gay and bisexual) do not benefit from this indirect protection, and so up to the age of 45.
Some transgender people can also get the vaccine.
Those assigned female at birth would have gotten one as a child. But those assigned male at birth could get a jab if they transition to female and have sex with men.