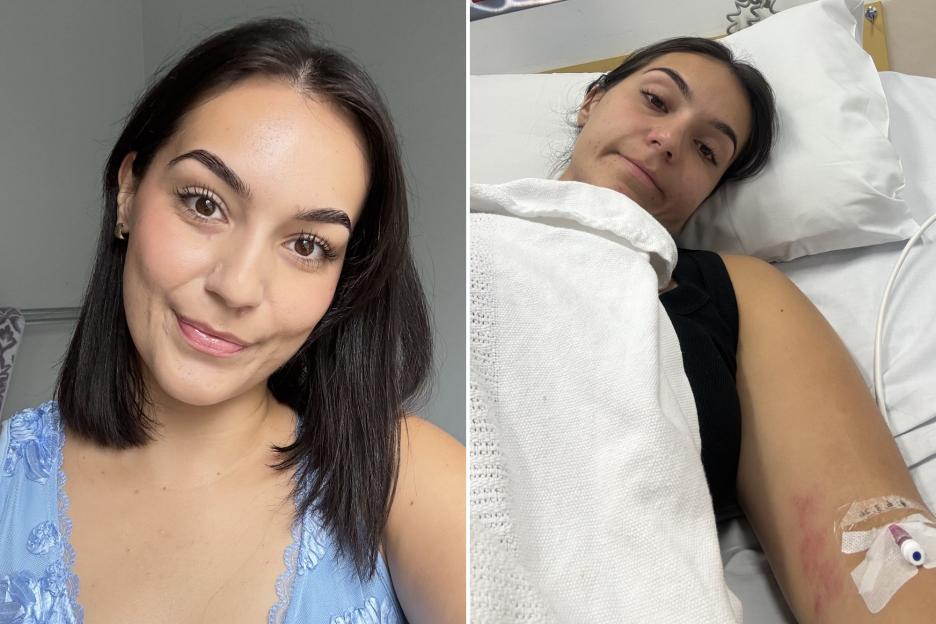
WHEN it came to work drinks, Steve Roe prided himself on always being the “last man standing”, seeking out that “one last drink” at any cost but leaving him covered in mystery bruises, and plunging him into dark, depressive states.
By 2012, had taken over the 42-year-old’s entire life and no amount of therapy, rehab or AA could fix it – until a simple pill has “saved” his life.
 Steve Roe says his issues with alcohol started young, when he’d drink mostly pints of lager but wash them down with shots Credit: Supplied
Steve Roe says his issues with alcohol started young, when he’d drink mostly pints of lager but wash them down with shots Credit: Supplied
 By the time he reached 42, alcohol had taken over his entire life Credit: Supplied
By the time he reached 42, alcohol had taken over his entire life Credit: Supplied
He’d rock up to work most Friday mornings fuzzy-headed after going hard on a Thursday night and would through until lunchtime when he would seek out “hair of the dog” to alleviate his hangover.
The advertising exec from Wolverhampton told Sun Health: “It was a work hard, play hard culture.
“Pretty much half, if not more, of my week involved heavy drinking.”
His issues with alcohol started young, when he’d drink mostly pints of lager but often wash them down with shots.
He says: “By the time I went to university in to study Media and Communications in 2002, I was regularly going out and not remembering how I got home.
“Sometimes I’d leave early, but I was often the last person standing, buying shots and being a bit of a drunken idiot.”
After landing his dream job and moving to London in his twenties, Steve says his issues with alcohol really started to ramp up.
“I worked in Soho, I was earning good , enjoying the London lifestyle, and ticking a lot of the boxes people aim for; career success and eventually buying a house,” he says.
But what started as weekend drinking, soon turned into weekday drinking, even though he was still managing to eat well and even on the days he wasn’t boozing.
“Despite my behaviour being pretty good when I wasn’t drinking, my relationship with alcohol just got worse,” he says.
“It wasn’t that I drank every day, just that when I did, I couldn’t stop.
“Friday lunch with colleagues would be four or five drinks, cocktails or gin and tonics, and then I’d continue drinking through the evening at the pub.
“I stopped properly counting drinks because I’d just given up trying to control it.”
Luckily, Steve never ended up in any serious trouble when he drank, but blacked out a lot.
“I would stay out later and later, looking for ‘one more drink’ with someone because I didn’t want to go home alone,” he says.
“Sometimes I’d end up with groups of people I barely knew.
“I’d wake up the next day not remembering how I got home, with bruises and terrible hangovers which were brutal.
“They completely destroyed me physically and mentally.”
When Steve’s started to be affected, he knew things had to change.
“By Saturday or Sunday I’d often fall into really dark, depressive states,” he says.
“I’d be stuck on the sofa, unable to move, feeling hopeless. I started to become more and more desperate for change.”
Steve had always dreamt of moving to one day.
So after a failed attempt at not drinking post-Covid, which saw his drinking spiral quickly again, he took the plunge, giving up his flat and career in advertising.
I didn’t know at the time, but my old friends in the UK and my new friends in Spain had contacted each other without me knowing. Everyone was incredibly worried
Steve Roe
“I thought if I moved to Spain, the change in environment would fix my drinking,” he says.
“Naively, I believed I’d adopt a more relaxed and Spanish relationship with alcohol, drinking slowly, having small beers, and enjoying it in moderation.
“But that’s not what happened.”
In Spain he tried to build a career as a , but had no routine, no real job yet, and very few friends.
He went out to meet people and his drinking spiralled even faster.
“After about six months I hit rock bottom,” he says.
“My family and friends all said I sounded drunk or severely hungover whenever they spoke to me.
“Eventually, they stepped in and brought me back to the UK for a stint in rehab.
“I didn’t know at the time, but my old friends in the UK and my new friends in Spain had contacted each other without me knowing.
“Everyone was incredibly worried about me.”
Steve started the 12-step program and , but it didn’t resonate with him.
 After a failed attempt at not drinking post-Covid, Steve left his life in the UK behind and moved to Spain Credit: Supplied
After a failed attempt at not drinking post-Covid, Steve left his life in the UK behind and moved to Spain Credit: Supplied
 After about six months of meetings, Steve left AA Credit: Supplied
After about six months of meetings, Steve left AA Credit: Supplied
“I felt like I couldn’t talk openly about my experience without being told I was ‘in denial’,” he says.
“For many people, AA works incredibly well, but for me it felt disempowering.
“When I returned to Spain and attended meetings there, I felt even more disconnected.
“I didn’t feel comfortable, but I also didn’t know what other options existed.
“It almost felt like a second rock bottom.”
AA, self-help, Dry Jan… NOTHING stopped me… until I found the Sinclair Method
Steve had already spoken to his , joined support groups, taken antidepressants for , and done and Sober October, but nothing seemed to help.
“I tried setting rules like only drinking on certain days,” he says.
“I read countless self-help books and listened to audiobooks.
“I spent a lot of money on therapy, talking therapies, trauma therapy, EFT tapping, and hypnotherapy, but almost all the approaches focused on finding a trauma that might explain my drinking.
“For me it was digging for something that simply wasn’t there. The more I searched for a trauma that didn’t exist, the more I felt like I was failing.”
After about six months of meetings, Steve left AA.
Are you drinking too much?
It is suggested that men and women should not drink more than 14 units of alcohol per week. That’s the equivalent of 6 pints of an average-strength beer, or 10 small glasses of a lower-strength wine.
The NHS suggests that someone may need help with their drinking if:
- They feel the need to drink alcohol
- Drinking alcohol is causing them to get into trouble
- They are warned by others about the amount of alcohol they consume
- They themselves believe their drinking is an issue
Drinking too much can lead to issues such as accidents requiring visits to hospitals, violent behaviour or losing your possessions in the short term. In the long term, alcohol misuse can lead to serious health risks such as heart disease, strokes, and a number of different types of cancer.
If you feel that you are drinking too much, the NHS suggests seeking advice from your GP and to be transparent about the extent of your drinking. However, if someone is hallucinating or experiencing severe tremors or seizures then they should call 999 as these are symptoms of severe alcohol withdrawal.
“At that point I remembered seeing a psychiatrist advertised online who was based in southern Spain,” he says.
“I had this strange instinct he could help, so I made an appointment.”
It was at that appointment that Steve learned about a protocol called the Sinclair Method and a drug known as the “Ozempic for alcoholics”.
“When he explained the neuroscience behind it, everything suddenly made sense,” says Steve.
is a pill that blocks the brain’s opioid receptors, which are responsible for the pleasurable ‘reward’ feelings alcohol normally triggers.
Taken about an hour before drinking, the medication gradually teaches the brain that alcohol doesn’t give the same reward, weakening the craving to drink.
Steve’s psychiatrist told him that whatever originally led him to drink wasn’t the main issue.
“The real problem was my brain had learned to associate alcohol with a powerful reward,” he says.
Over time, that reward loop had become too strong to break alone – but the drug might just manage it.
Steve started on Naltrexone and felt a change within days.
Although it took nine months for him to feel like his relationship with alcohol had fundamentally changed, he’s now three years in and the happiest he’s been in a long time.
“It has completely transformed my life and probably saved it,” he says.
 Steve started on Naltrexone and felt a change within days Credit: Supplied
Steve started on Naltrexone and felt a change within days Credit: Supplied
 It took nine months for him to feel like his relationship with alcohol had fundamentally changed Credit: Supplied
It took nine months for him to feel like his relationship with alcohol had fundamentally changed Credit: Supplied
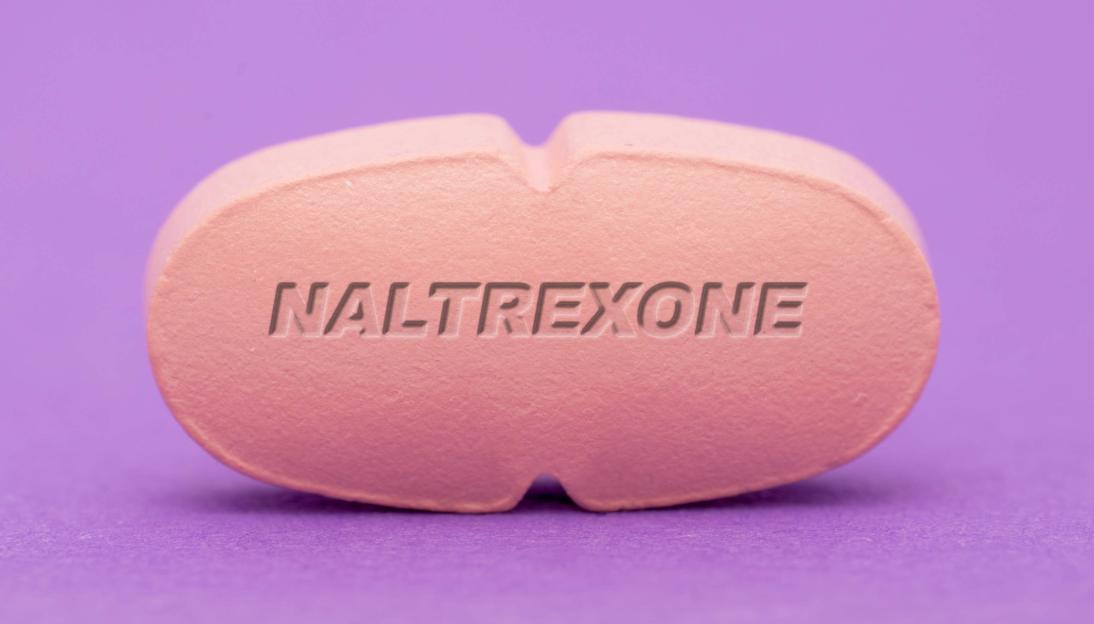 Naltrexone is a pill that blocks the brain’s opioid receptors, which are responsible for the pleasurable ‘reward’ feelings alcohol normally triggers Credit: Getty
Naltrexone is a pill that blocks the brain’s opioid receptors, which are responsible for the pleasurable ‘reward’ feelings alcohol normally triggers Credit: Getty
Once he’d reached a stable point with booze, he decided he wanted to raise awareness of the Sinclair Method.
“I realised how many people like me are stuck in the middle,” he says.
“They know alcohol is a problem but don’t feel that traditional recovery paths fit them.”
Steve now works with a charity that raises awareness of the Sinclair Method, called Options Save Lives , and is a coach with Rethink Drink .
“People can reach out to me through social media or through the coaching work I do,” he says.
“It took me years to find the right solution for me but if I could speak to my younger self, I’d say: trust your instincts.
“Walking away from AA was difficult because it works for so many people, but trusting them is what led me to the solution that saved my life.”
Steve also has advice for anyone struggling with alcohol.
“It’s not always as black and white as ‘drink normally’ or ‘quit forever’,” he says.
“The Sinclair Method gave me control over alcohol again.
“No one should have to reach rock bottom before discovering this option exists.”
What is the Sinclair Method?
The Sinclair Method utilises the body’s nervous system to remove a person’s interest in consuming alcohol and the behaviour surrounding it.
A dependence on alcohol isn’t simply about withdrawal from alcohol.
The process of alcohol drinking is a behaviour someone learns, and every time they drink alcohol, this behaviour is reinforced through the brain’s opioid system, say researchers.
Quitting drinking alcohol can be harder for some individuals due to factors such as their genetics and if their behaviours are repeatedly reinforced.
The Sinclair Method differs from other methods because, instead of encouraging people to just go cold turkey, it helps eliminate the craving for alcohol completely.
It says on the website: “When you drink often, your brain learns: alcohol = reward. When you stop suddenly, your brain feels deprived of a reward it still expects. And the longer you go without alcohol, your brain may still be wired the old way, so it keeps sending strong ‘wanting’ signals.
“To change that wiring, the brain has to learn a new lesson: alcohol does not deliver the same reward anymore. That unlearning is called extinction. Pharmacological extinction is when the reward is blocked during drinking sessions, so over time the brain can weaken the link between alcohol and craving.”
Using opioid antagonists (like the medicine naltrexone), it triggers the ‘extinction mechanism’ in the brain. This results in an individual’s craving for alcohol to reduce, as well as how much they drink too.
Naltrexone blocks the brain’s opiod receptors that release endorphins that create a buzz when someone drinks. It removes the feel-good association (or ‘reward loop’) with booze.
The tablet is taken one hour before planned drinking.
HOW IT WORKS:
Step 1:
- Book a consultation with a clinician
- They will see if The Sinclair Method is the right fit for you
Step 2:
- If The Sinclair Method is the right path, then you will be prescribed an opioid blocker. This is what stops the feeling of being ‘rewarded’ by alcohol.
Step 3:
- After starting the medication, you can continue to drink in ‘normal circumstances’, but must take the opioid blocker. In one or two weeks, youll notice shifts in how you feel when drinking.
Step 4:
- By weeks three to six cravings begin to reduce and you will feel less of an urge to drink.
Step 5:
- You will feel more in control of your drinking. In weeks seven and more, the reinforcement with alcohol is weakened and some may choose to stop drinking altogether, while others maitain moderation.