GEMMA Doherty visited her GP and A&E at least eight times, distressed by her symptoms.
But time and time again, she claims she was told she was “fit and well”, and “too young for cancer” – despite suffering so severe she was soaking through clothes and the sofa.
 Gemma claims she was told she was ‘too young’ for cancerCredit: SWNS
Gemma claims she was told she was ‘too young’ for cancerCredit: SWNS
 Then she was diagnosed with cervical cancerCredit: SWNS
Then she was diagnosed with cervical cancerCredit: SWNS
The mum says bungling dismissed her with “stress and hormones”.
The 39-year-old, from Derby, was eventually found to have a satsuma-sized lump on her cervix, meaning she had .
And doctors said it was inoperable, meaning they have to use and to try and shrink it.
Gemma has been left house-bound and forced to give up her day job in sales while she battles the tumour.
She needs help with daily jobs and is unable to cook or clean up unaided.
“It’s just frustrating that you go to a GP and you have faith in them, but you don’t get taken seriously,” Gemma tells Sun Health. “It’s pigeonholing me into a set of beliefs.”
Furious, Gemma says her smear tests had been clear for years – her last one was in April 2024.
Smear tests look for , which is a virus that can lead to .
The tests, given to women every five years – or more often, if there is HPV – can also find abnormal changes to the cervix.
Gemma, who used to work in marketing and sales, said she’d been having her smear test every five years and says nothing abnormal was detected.
“The type of cancer I’ve been diagnosed with is an HPV cancer that should have shown up on the smear test,” she says.
“Smear tests only test for HPV and not cancer. I had no idea this was the case.
“How many women are walking around with cancer after being told their smear test is all clear?”
“I don’t want another woman to ignore symptoms just because they’ve got a clear smear. Early action saves lives.”
Gemma had symptoms and started seeing her GP in September last year.
 She was feeling rough and tired and bleed through her clothesCredit: SWNS
She was feeling rough and tired and bleed through her clothesCredit: SWNS
 Gemma had to go to hospital to get a diagnosisCredit: SWNS
Gemma had to go to hospital to get a diagnosisCredit: SWNS
 Two days later, the team ordered an urgent biopsy and then an urgent MRI scan.Credit: SWNS
Two days later, the team ordered an urgent biopsy and then an urgent MRI scan.Credit: SWNS
She had started to suffer with heavy bleeding which soaked her sofa and clothes and left her house-bound.
But doctors at her local Lister House Surgery in Oakwood and Chellaston reckoned it was caused by hormones and stress – despite numerous visits.
Gemma said: “I had some really severe bleeding that wasn’t a period or usual for me. It was clotted and it was bad. It was on and off.
“It was day to day, it was unpredictable.
“I could be on the sofa or bed, out and about, it was purely unpredictable.
“I didn’t have bleeding during intimacy, it was day-to-day. It was heavy and bright red, it was like someone had cut me internally.
“I would pull my underwear down and there would be blood everywhere.
“I went to the GP, they said I’m too young for cancer and I’m fit and well.”
Gemma says she had four internal speculum examinations at Lister House Surgery in Oakwood between October and November last year.
When doctors had no concerns, Gemma says: “They said it was hormonal, stress or perimenopausal. They were having none of it.
“I kept on going back because I knew something was wrong.
“They said my cervix was normal, there weren’t any abnormalities. Then I got more severe pain, I was feeling rough and tired.
“I was quite bad, I got ill quite quickly. They did tests and they said everything looked okay into November.
“I knew something was off. You know your own body.”
Gemma was referred to gynaecology, but the wait was 20 weeks.
Who's at risk of cervical cancer?
Nearly all cervical cancers are caused by an infection with certain high-risk types of human papillomavirus (HPV).
HPV is the name for a very common group of viruses that most people will get some type of HPV during their lives.
It’s very common and nothing to feel ashamed or embarrassed about.
You can get HPV from any kind of skin-to-skin contact of the genital area, not just from penetrative sex.
This includes:
- Vaginal, oral or anal sex
- Any skin-to-skin contact of the genital area
- Sharing sex toys
In most cases your body will get rid of HPV without it causing any problems.
But sometimes HPV can stay in your body for a long time and some types of high risk types of HPV can cause cervical cancer.
If high risk types of HPV stay in your body, they can cause changes to the cells in your cervix. These changes may become cervical cancer if not treated.
How to lower your risk of cervical cancer
You can’t always prevent cervical cancer. But there are things you can do to lower your chances of getting cervical cancer.
Cervical screening and HPV vaccination are the best ways to protect yourself from cervical cancer.
- All women and people with a cervix between the ages of 25 and 64 are invited for regular cervical screening . It helps find and treat any changes in the cells of the cervix before they can turn into cancer.
- All children aged 12 to 13 are offered the HPV vaccine . It helps protect against the types of HPV that cause most cases of cervical cancer, as well as some other cancers and genital warts.
You can also lower your chance of getting cervical cancer by:
- Using condoms, which lower your chance of getting HPV – but they do not cover all the skin around your genitals so you’re not fully protected
- Quitting smoking – smoking can weaken your immune system and the chemicals in cigarettes can also cause cervical cancer
Source: NHS
“They didn’t put me on an urgent referral like I asked them to,” she says. “They put me on a 20-week wait.
“My first appointment would be the middle of January if I’d waited.
“I couldn’t leave the house, it was going through my underwear, pads, clothing, on my sofa. I couldn’t cope.”
Frustrated with the constant bleeding and worsening pain, on November 26, Gemma decided to wait in her local gynaecology ward at Royal Derby Hospital and force staff to do a proper check.
“I took myself off to the gynaecology ward and presented myself,” says Gemma.
“I sat there for five hours and eventually got seen.
“The doctor had a look and found a mass straight away. He said there is something that they needed to look at.”
Two days later, the team ordered an urgent biopsy and then an urgent MRI scan.
“But I just knew,” says Gemma.
“On December 19 I went back with my mum and I was telling her that I knew it was going to be bad news.
“They told me it was cervical cancer, stage 1, B3 and confined to my cervix.
“The tumour was quite big at 5cm, around the size of a satsuma.”
Doctors had found a satsuma-sized tumour, which was revealed to be stage 1 B3 cervical cancer
Gemma is now facing weeks of gruelling chemotherapy and radiotherapy.
Due to the position of the tumour – next to her bladder and bowel – doctors aren’t able to operate.
 The mum is now aiming to raise cancer awareness after living with an undetected tumour.Credit: SWNS
The mum is now aiming to raise cancer awareness after living with an undetected tumour.Credit: SWNS
 The treatment used to shrink the tumour also destroyed her ovaries meaning she is now infertile due to induced “medical menopause”Credit: SWNS
The treatment used to shrink the tumour also destroyed her ovaries meaning she is now infertile due to induced “medical menopause”Credit: SWNS
Single Gemma added: “It’s the stigmatism for my age, I’ve had to advocate for my age and tell them what I need.
“I’ve had to do their jobs for them. It shouldn’t be like that, I went to them enough times.
“It’s also the frustration. If I waited, there is no way I would be in treatment right now.
“I was in hospital most of January, I was having severe bleeds to the point of collapse.
“I had a bleed in A&E, and they just sat there while I bled on the floor. It’s not dignified.
“I’ve had three blood transfusions because of all of the blood I’ve lost. My body couldn’t cope with the amount I’ve lost.”
The treatment used to shrink the tumour also destroyed her ovaries meaning she is now due to induced “medical menopause”.
“My ovaries are dying,” she says.
“My children are 12 and 16, but it’s an awful thing to have to endure earlier than you otherwise should.
“They’re saying it’s 80 to 90 per cent curable, but everyone is different. We’ve had our hiccups.
“I’ve been housebound, to the point where I’ve had to ask people to cook and clean for me and help me get ready.
“I’ve had to get people to drive me to hospital.”
Gemma’s friend has set up a GoFundMe to help her with bills while she endures her treatment.
Gemma says: “My friends set up a GoFundMe to help a little bit. It’s not about the money, it’s about getting the message out there.
“I’d love to raise some awareness about young women and smears.
“Clear smears don’t mean you haven’t got cancer. If you’ve got symptoms, please go and get them checked out.
“It’s important to me to get the message out there to as many people as possible. I never thought it’d be me having this, but it is.”
NHS Derby and Derbyshire Integrated Care Board, which supports Lister House Surgery, refused to comment.
A spokesperson said: “I’m sorry but the practice cannot comment on an individual case, because of its need to protect patient confidentiality.
“The practice has an absolute duty of confidentiality to its patient.”
How to protect yourself against cervical cancer
CERVICAL cancer is most commonly diagnosed in women in their early 30s, with around 3,200 new cases and 850 deaths each year in the UK.
According to CRUK, the five-year survival rate is around 70 per cent – and the earlier it is caught, the better.
Cervical screening programmes and HPV vaccines have reduced rates and save 4,000 lives each year.
It is vital you attend your smear test and get jabbed when invited, and that you know the symptoms of cervical cancer to look out for.
These aren’t always obvious, and they may not become noticeable until the cancer has reached an advanced stage.
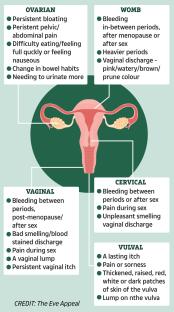
But you might notice:
- Unusual bleeding (often after sex, between periods, or after the menopause)
- Pain and discomfort during sex
- Vaginal discharge (often unpleasant smelling)
- Pain in your lower back, between your hip bones or in your lower tummy
Women are invited to have regular cervical screenings between the ages of 25 and 64. How often depends on your age.
The HPV vaccine, which helps protect against the virus, is recommended for children aged 12 to 13 and people at higher risk from HPV.
Source: NHS and Cancer Research UK






