WHEN Julie Hughes woke up from a deep coma, she couldn’t remember Scott – her husband and the father of her two kids.
Only two weeks before, he had been by her side as she writhed around in pain, vomiting poo, her bowel destroyed by a disease that had been left misdiagnosed by GPs for years.
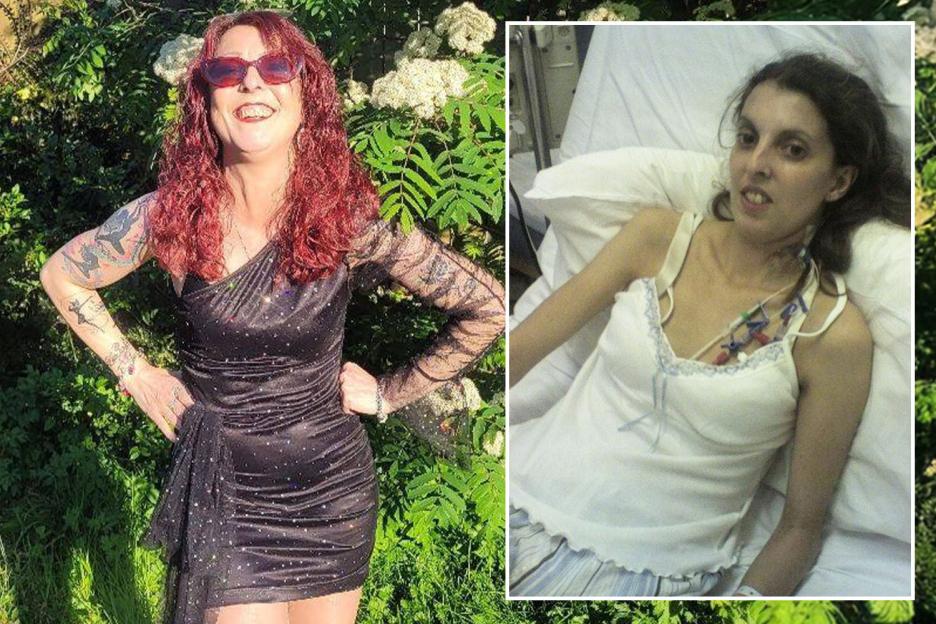
 Mum-of-two Julie Hughes, 51, almost died after years of IBS-like symptomsCredit: Supplied
Mum-of-two Julie Hughes, 51, almost died after years of IBS-like symptomsCredit: Supplied
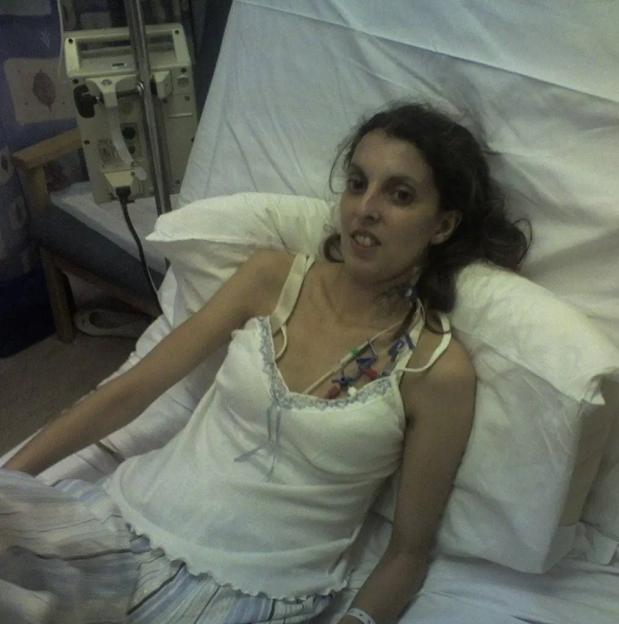 Her ordeal came to a head in 2006, when she was hospitalised. Nothing she ate was being absorbed, with “various expulsions of fluids from both ends”Credit: Supplied
Her ordeal came to a head in 2006, when she was hospitalised. Nothing she ate was being absorbed, with “various expulsions of fluids from both ends”Credit: Supplied
Julie had , her pulse stopped, and her life hung in the balance. Her family were told to say their goodbyes while she lay in a coma.
“My family went through absolute hell, wondering whether I would ever be their ‘Julie’ again, or whether I would even survive,” Julie, now 51, who lives in Clydebank in , tells Sun Health.
“I vividly remember living eleven bizarre, very real coma lives during those two weeks of unconsciousness.
“When I woke up, I was completely confused and could not even remember being married to Scott. At that point, we had been married three years and had been together since I was 18.
“I didn’t know my own age, and I thought I was still a teenager.”
It was when she was a teenager that her ordeal began – leading up to the near-death experience when she was 31 years old.
Stomach pain, diarrhoea and fatigue – doctors kept telling her that she had (IBS).
Julie, who fosters abused and neglected dogs, says: “Despite countless visits to my GP, my symptoms were repeatedly dismissed as IBS.”
Her symptoms worsened when she had her first child, Kyle, aged 20, in 1994, and she dropped down to six stone.
Julie says: “I found myself constantly going back and forth to the doctors. Investigations were carried out, but I was only prescribed more medication.”
It wasn’t until 2000, when she was 25, that was finally considered, because a lump was found in her stomach during her second pregnancy.
to IBS, but they are different.
IBS is a common condition, affecting up to one in ten, in which the bowel doesn’t function properly. It may be triggered by foods, stress or hormones.
is related to a fault in the immune system and is classified as a disease, rather than a syndrome of symptoms, like IBS.
The inflammation – which can occur anywhere in the gut, from the mouth to the bottom – damages the bowel and is much more likely to cause hospitalisation and complications, while increasing the risk of
Crohn’s and colitis (another inflammatory bowel disease/IBD) affects 500,000 people, or one in 123 people, according to the charity Crohn’s and Colitis UK .
It had taken seven years for Julie to get a diagnosis of Crohn’s – but unfortunately, it was only the start of her misery.
What is Crohn's disease?
CROHN's disease is a lifelong condition where parts of the digestive system become inflamed.
It is a type of inflammatory bowel disease (IBD) which, along with ulcerative colitis, affects almost half a million people in the UK.
Symptoms usually start in childhood, but the disease affects people of all ages. These include:
- Diarrhoea
- Stomach aches and cramps
- Blood in your poo
- Tiredness (fatigue)
- Weight loss
There is no cure, but treatment can help reduce or control symptoms.
Some people take medication to lessen inflammation in the digestive system, while others might have surgery to remove a small area.
The exact cause is unknown, but genes, problems with your immune system, smoking, stomach bugs and gut bacteria imbalances are believed to play a part.
Source: NHS
Julie says: “The next five years were incredibly painful. I was juggling extreme exhaustion, severe weight loss, endless trips to the toilet, and constant, excruciating pain, all while trying to be a good mum.”
She was also studying Art and Design while dealing with frequent flare-ups and accidents, and remembers “embarrassing memories that still stay with me today”.
My family were unsure if I was going to live or if I was going to be mentally disabled
Julie Hughes
“One time I remember I was standing outside college with friends when suddenly I felt my bowels open,” she recalls.
“I could not control it and they burst out onto my underwear. The hobble to the toilets felt unending.
“I sat there until I knew the classes had resumed then escaped, running quickly out of the building, heading for home.”
Julie was admitted to hospital several times throughout June and July of 2006 with “crushing” lethargy and sickness.
“If I did manage to eat, I just spewed it back up,” she says. “The pain was excruciating at times.”
Close to death
On August 3, 2006, when she was 31, Julie ended up in A&E – “nearly for the last time”, she recalls.
“I lay writhing in agony on the floor. I could smell poo, and after asking my husband, we realised I was vomiting it… as well as experiencing .
“I didn’t know it then, but I was close to death.”
At this point, Julie had a bowel fistula – when a tunnel forms between two organs, which can lead to serious infection due to the leaking of fluids.
She also had stricture – narrowing of the intestine.
“I could not absorb anything, my body was losing vital vitamins and minerals due to the various expulsions of fluids from both ends,” says Julie.
“The blockage in my gut was stopping waste from passing through properly, causing vomiting containing faecal matter, hence the smell of poo.
“I was very close to, or had, . From that point on, my memories become hazy.
“My family were called and told to prepare for the worst — to come and say goodbye.”
Doctors performed two emergency surgeries and cut any damaged or diseased part of her bowel out.
She then fell into a coma while her mum, sister, Louise, 46 and husband, Scott, 56, waited by her bedside.
 Julie now lives with just 100cm of bowelCredit: Supplied
Julie now lives with just 100cm of bowelCredit: Supplied
 Her condition is stable, thanks to medicationCredit: Supplied
Her condition is stable, thanks to medicationCredit: Supplied
“My family were unsure if I was going to live or if I was going to be mentally disabled,” Julie says.
When Julie woke up, she discovered that she had – a pouch outside the body which collects waste (poo) from a tube connected to the intestine.
She was dependent on liquid food via IV for almost two years, so that it would bypass her bowel.
Living with a stoma isn’t easy and Julie experienced a number of embarrassing incidents in which her stoma bag burst.
One time, was when they visited a family member who had just had babies.
“I was sat with one little lad when there was a disgusting smell,” Julie recalls. “I jokingly exclaimed, ‘oops, somebody needs a nappy change!’
“However, I soon realised the smell was from me. My stoma bag had burst (a horribly regular occurrence). I quickly made an excuse and ran to my car crying.
“There were multiple times when I soiled our marital bed, it made me feel disgusting and so embarrassed, it crushed me,” she says.
“Scott was so good though, he cleaned me up as well as changing the covers.”
Thankfully, Julie was able to have her stoma reversed in 2007, and in the years since, she has learned to live with a significantly smaller bowel than everyone else.
She says: “Only having 100cm of bowel left means I cannot absorb the nutrients my body needs to function properly which can cause problems, especially the fatigue.
“I still experience an extremely painful abdomen and have diarrhoea at least five times per day, depending on what I eat or drink.
“It is affecting my joints and crushing fatigue takes over so often. However, I am on medication that seems to be keeping it fairly stable.”
Julie wants to raise awareness of Crohn’s and colitis, so more people recognise the symptoms earlier and get the help they need sooner.
“I also want to share hope, to remind people that strength can be found, even in the darkest times, even if it takes time,” she says.
“I have Crohn’s, but Crohn’s does not have me.”